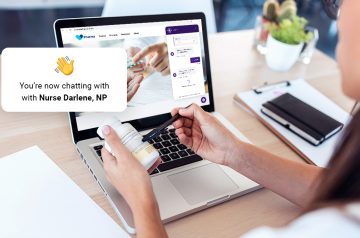
The first patient-centered, nurse powered EMR for telemedicine Digital health programs require a patient experience that proactively engages patients and helps them navigate through the healthcare process. This is why...
all content
Patient Support Services and Pharma Omnichannel Strategies
In the ever-evolving landscape of healthcare, pharmaceutical manufacturers are facing a critical imperative: to redefine and elevate the patient and customer experience. As consumers increasingly demand seamless and effortless interactions, the...
A Nurse’s Guide to Weight Loss with Semaglutide: Wegovy®, Ozempic®, and Rybelsus®
Hi there! Nurse Kim here, and today I want to talk to you about something amazing called Semaglutide. It might sound like a big word, but don’t worry, I’m here to...
It’s Time to Put Patient Support at the Center of Digital Healthcare
Live chat – built specifically for pharma – can help companies offer better patient education and more efficient escalation. The next wave of nursing transformation is underway. Digital patient support is...
Highlighting Our Heroes: Kate Murphy, CNM
Spotlighting another amazing Nurse-1-1 nurse who is providing empathy and trust for patients within digital health websites. When you embed a nurse live chat into your digital health or online pharma...
Not Your Average Live Chat: How Nurse-1-1’s Unique HIPAA-Compliant Live Chat Increases Security and Patient Trust
A HIPAA-compliant live chat is essential for your digital health or pharma website. Live chat is a great way to engage patients when they’re already browsing your website – i.e. when...
Nursing Looks Different – But It’s Still the Key To Patient Engagement and Adherence
A veteran nurse’s perspective on her profession’s changing role – and how nurse live chat can drive better patient outcomes and increase revenue for digital health platforms. The next wave of...
Who Are the Nurse-1-1 Nurses?
Despite being digital, our nurses still embody safety, empathy and trust throughout patients’ healthcare journeys. While we have almost three thousand nurses on the front lines of digital heath, our front...
Highlighting Our Heroes: Catherine & Nicole
Spotlighting two of our amazing Nurse-1-1 nurses on the front lines of digital healthcare, providing empathy and trust for patients. Picture this: a patient is logged onto your digital health or...
Patient Engagement is the Key to Better Health Outcomes
Digital health and online platforms can educate and influence patients to make the best healthcare decisions, improving relationships and increasing revenue along the way. Healthcare looks very different from the past,...
Dear Digital Healthcare: Let’s Do Better
Digital transformation has increased healthcare access, but quality and consistency are lagging behind. A human touch – and some innovative thinking – can get us where we need to be. Michael...